Monireh Rahimkhani; Zahra Rajabi; Seyed Saeed Alavi fard; Shokoofeh Akbari; Manijeh Aliasghar
Abstract
Staphylococcus aureus (S. aureus) is an important pathogen that is involved in causing various infections. The most important problem in the treatment of staphylococcal infections is ...
Read More
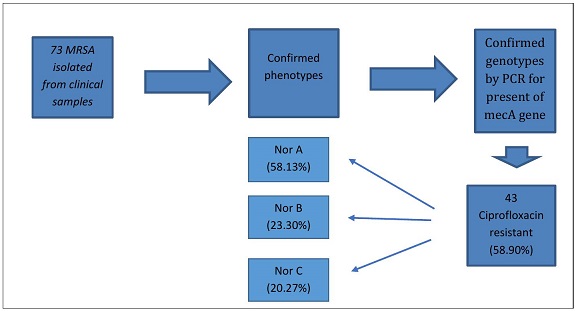
Staphylococcus aureus (S. aureus) is an important pathogen that is involved in causing various infections. The most important problem in the treatment of staphylococcal infections is the increasing drug resistance of these bacteria. In this research, the presence of efflux pump genes in methicillin-resistant Staphylococcus aureus strains isolated from clinical samples was investigated. 73 MRSA were collected and confirmed phenotypically and biochemically. PCR was performed by checking the presence of mecA, vanA, norA, norB, and norC genes. All 73 clinical samples underwent meticulous confirmation, unequivocally establishing their classification as Methicillin-Resistant Staphylococcus aureus (MRSA). Delving into the antibiotic resistance landscape, a substantial portion of the MRSA strains (58.90%) manifested resistance to ciprofloxacin, with the norA gene emerging as the predominant contributor in 25 instances (58.13%). Frequency of vanA genes among isolated MRSA was 5 (6.84%). Furthermore, a nuanced genetic complexity was unveiled as certain MRSA isolates exhibited the presence of all three norA, norB, norC genes concurrently, or alternatively, the co-occurrence of two among them. This intricate molecular profile accentuates the multifaceted nature of antibiotic resistance mechanisms within the MRSA population under scrutiny, underscoring the need for a comprehensive understanding to inform targeted therapeutic interventions. The presence of vanA and efflux pump resistance genes among the studied isolated MRSA is a warning for the spread of MDR strains in clinical isolates. This current study further underscores the peril associated with such infections within hospital systems. Given the elevated clinical significance of these infections, it becomes imperative to prioritize the awareness of healthcare professionals. Consequently, enhancing the vigilance and preparedness of medical practitioners becomes paramount in addressing the evolving landscape of antimicrobial resistance within healthcare settings.